Serum and epidermal levels of sphingosine 1-phosphate (S1P) are higher in patients with psoriasis than healthy subjects. Although roles of type 1 S1P receptor, S1P1, in the development of psoriasis has intensively been investigated, roles of S1P2 have not been elucidated. We aim to investigate whether blockage of S1P2 reduce imiquimod-induced psoriasis-like dermatitis using an S1P2 antagonist, JTE-013, in combination with S1pr2 wild-type (WT) and knock-out (KO) BALB/c mice. Imiquimod induced increase of erythematous papules and plaques with silver scaling, whereas administration of JTE-013 significantly suppressed those increases in S1pr2 WT mice. Deficiency of S1pr2 gene reduced the imiquimod-induced symptoms. Imiquimod increased mRNA expression levels of pro-inflammatory Th1/Th17 cytokines, whereas JTE-013 significantly suppressed those increases in S1pr2 WT mice. Deficiency of S1pr2 gene also suppressed the imiquimod-induced pro-inflammatory cytokine expression. Imiquimod induced enlargement of lymph nodes and spleens, whereas JTE-013 suppressed them in S1pr2 WT mice. Imiquimod induced increase of pro-inflammatory Th1/Th17 cytokine levels and Th17 cell numbers in lymph nodes and spleens, whereas JTE-013 suppressed them in S1pr2 WT mice. In summary, the present results suggest that blockage of S1P2 could suppress the characteristics of psoriasis-form dermatitis and be a therapeutic strategy.
In Biomolecules Therapeutics on 1 May 2025 by Lee, J. H. & Im, D. S.
In International Journal of Molecular Sciences on 13 December 2024 by Lee, J. H., Lee, J. E., et al.
The amount of sphingosine 1-phosphate (S1P) found in the synovial tissue of individuals with rheumatoid arthritis is five times greater than that in those with osteoarthritis. Our study aims to determine whether inhibiting S1P2 can mitigate collagen-induced rheumatoid arthritis (CIA) by using an S1P2 antagonist, JTE-013, alongside DBA-1J S1pr2 wild-type (WT) and knock-out (KO) mice. CIA causes increases in arthritis scores, foot swelling, synovial hyperplasia, pannus formation, proteoglycan depletion, cartilage damage, and bone erosion, but these effects are markedly reduced when JTE-013 is administered to S1pr2 WT mice. CIA also elevates mRNA expression levels of pro-inflammatory Th1/Th17 cytokines in the foot and spleen, which are significantly decreased by JTE-013 in S1pr2 WT mice. Additionally, CIA raises Th1/Th17 and Treg cell counts, while JTE-013 reduces these elevations in the spleens of S1pr2 WT mice. Treatment with JTE-013 or the absence of S1pr2 curtails the differentiation of naïve T cells into Th1 and Th17 cells in a dose-dependent manner. In SW982 human synovial cells, JTE-013 lowers LPS-induced increases in pro-inflammatory cytokine levels. Overall, these findings propose that blocking S1P2 in immune and synovial cells may alleviate rheumatoid arthritis symptoms and offer a potential therapeutic approach.
In Frontiers in Immunology on 11 October 2024 by Masuda-Kuroki, K., Alimohammadi, S., et al.
Psoriasis is an inflammatory skin condition where immune cells play a significant role. The importance of the cross-talk between keratinocytes and immune cells in the pathogenesis of psoriasis has recently been reaffirmed. Recent studies have found that several S1PR functional antagonists, other than S1PR2, are effective in improving psoriasis. This study aims to investigate the role of S1PR2 in psoriasis, that has not been investigated before.
Spatial transcriptomics, RT-qPCR, and flow cytometry were used to map the immune cell landscape and its association with metabolic pathways in an imiquimod (IMQ)-induced psoriasis-like inflammation in S1pr2fl/fl K14-Cre mice that could not sense sphingosine-1-phosphate (S1P) in the epidermis through the S1PR2 receptor.
Our analysis suggests that S1PR2 in keratinocytes plays a major role in psoriasis-like inflammation compared to other S1PRs. It acts as a down-regulator, inhibiting the recruitment of Th17 cells into the skin. In IMQ-induced psoriasis skin, both S1pr2-/- and S1pr2fl/fl K14-Cre mice showed higher expressions of proinflammatory cytokines such as TNF-α, IL-17A, and IL-1β together with higher expressions of MyD88/NF-κB pathway compared to the wild-type mice. Remarkably, in IMQ-treated mice, the deletion of S1pr2 in keratinocytes only resulted in a larger population of Th17 cells in skin-draining lymph nodes. Other S1PR modulators did not improve the worsening of psoriasis-like inflammation caused by S1PR2 deficiency in keratinocytes.
This study reaches two main conclusions: signals from keratinocytes play a central role in creating an immune environment that promotes the development of psoriasis, and stimulating S1PR2, instead of suppressing it, represents a potential therapeutic approach for psoriasis.
Copyright © 2024 Masuda-Kuroki, Alimohammadi, Lowry and Di Nardo.
In Cell Communication and Signaling : CCS on 30 September 2024 by Fang, C., Ren, P., et al.
Mitochondria play a crucial role in shaping the macrophage inflammatory response during bacterial infections. Spinster homolog 2 (Spns2), responsible for sphingosine-1-phosphate (S1P) secretion, acts as a key regulator of mitochondrial dynamics in macrophages. However, the link between Spns2/S1P signaling and mitochondrial functions remains unclear.
Peritoneal macrophages were isolated from both wild-type and Spns2 knockout rats, followed by non-targeted metabolomics and RNA sequencing analysis to identify the potential mediators through which Spns2/S1P signaling influences the mitochondrial functions in macrophages. Various agonists and antagonists were used to modulate the activation of Spns2/S1P signaling and its downstream pathways, with the underlying mechanisms elucidated through western blotting. Mitochondrial functions were assessed using flow cytometry and oxygen consumption assays, as well as morphological analysis. The impact on inflammatory response was validated through both in vitro and in vivo sepsis models, with the specific role of macrophage-expressed Spns2 in sepsis evaluated using Spns2flox/floxLyz2-Cre mice. Additionally, the regulation of mitochondrial functions by Spns2/S1P signaling was confirmed using THP-1 cells, a human monocyte-derived macrophage model.
In this study, we unveil prostaglandin E2 (PGE2) as a pivotal mediator involved in Spns2/S1P-mitochondrial communication. Spns2/S1P signaling suppresses PGE2 production to support malate-aspartate shuttle activity. Conversely, excessive PGE2 resulting from Spns2 deficiency impairs mitochondrial respiration, leading to intracellular lactate accumulation and increased reactive oxygen species (ROS) generation through E-type prostanoid receptor 4 activation. The overactive lactate-ROS axis contributes to the early-phase hyperinflammation during infections. Prolonged exposure to elevated PGE2 due to Spns2 deficiency culminates in subsequent immunosuppression, underscoring the dual roles of PGE2 in inflammation throughout infections. The regulation of PGE2 production by Spns2/S1P signaling appears to depend on the coordinated activation of multiple S1P receptors rather than any single one.
These findings emphasize PGE2 as a key effector of Spns2/S1P signaling on mitochondrial dynamics in macrophages, elucidating the mechanisms through which Spns2/S1P signaling balances both early hyperinflammation and subsequent immunosuppression during bacterial infections.
© 2024. The Author(s).
In Advances in Radiation Oncology on 1 September 2024 by Miura, T., Kado, J., et al.
There is still no effective treatment for the gastrointestinal side effects of radiation therapy. Multilineage-differentiating stress-enduring (Muse) cells are tissue stem cells that have the ability to spontaneously home in on injured tissues and repair them. Several clinical trials have shown that stem cell therapy using human bone marrow-derived Muse (hBM-Muse) cells is effective in treating various diseases, but it is not known whether they are effective in treating radiation-induced intestinal injury. In this study, we investigated whether hBM-Muse cells are homing to the radiation-damaged intestine and promote its repair.
hBM-Muse cells were injected into the tail vein of mice 2 hours after high-dose total body irradiation. Then, homing analysis, crypt assay, bromodeoxyuridine assay, Terminal deoxynucleotidyl transferase-mediated deoxyuridine triphosphate nick end labeling (TUNEL) assay, immunostaining, and survival time measurements were performed. In addition, we analyzed the expression of sphingosine monophosphate (S1P), a Muse cell-inducing factor, in the mouse small intestine after irradiation. Finally, we investigated whether the administration of JTE-013, an S1P receptor 2-specific antagonist, inhibits hBM-Muse cells homing to the injured intestine.
S1P expression increased in mouse intestine after irradiation, with hBM-Muse cells homing in on the injured intestine. Injection of hBM-Muse cells after radiation exposure significantly increased the number of crypts, proliferating cells in the crypts, and small intestinal component cells such as intestinal stem cells inhibited radiation-induced apoptosis and prolonged mouse survival. Treatment with JTE-013 significantly inhibited intestinal homing and therapeutic effects of hBM-Muse cells. These findings indicate that hBM-Muse cells homed in on the injured intestine through the S1P-S1P receptor 2 interaction to exert therapeutic effects on the radiation-induced intestinal injury.
This study indicates that hBM-Muse cells are effective in treating radiation-induced intestinal injury, suggesting that hBM-Muse cell-based stem cell therapy has the potential to overcome gastrointestinal side effects that limit the indications for radiation therapy.
© 2024 The Author(s).
In Cell Commun Signal on 30 September 2024 by Fang, C., Ren, P., et al.
Fig.7.E
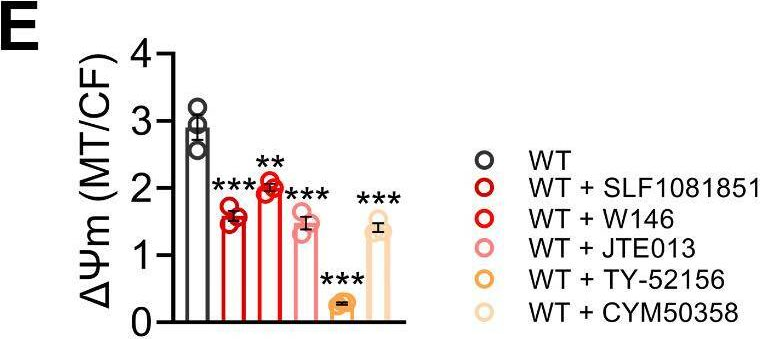
Collected and cropped from Cell Communication and Signaling : CCS by CiteAb, provided under a CC-BY license
Image 1 of 6
In Cell Commun Signal on 30 September 2024 by Fang, C., Ren, P., et al.
Fig.7.B
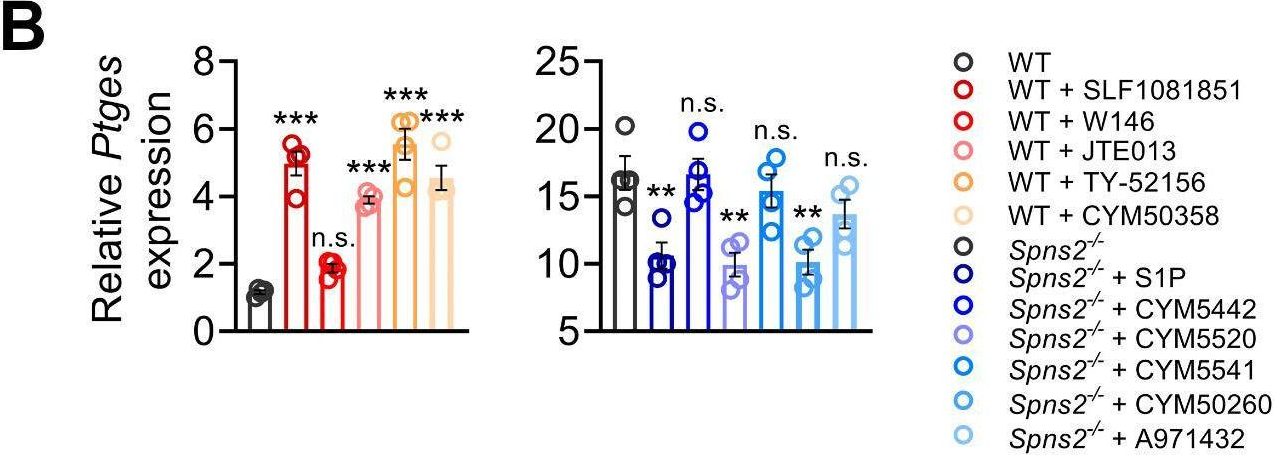
Collected and cropped from Cell Communication and Signaling : CCS by CiteAb, provided under a CC-BY license
Image 1 of 6
In Cell Death Dis on 1 March 2023 by Yang, S., Chang, N., et al.
Fig.7.G
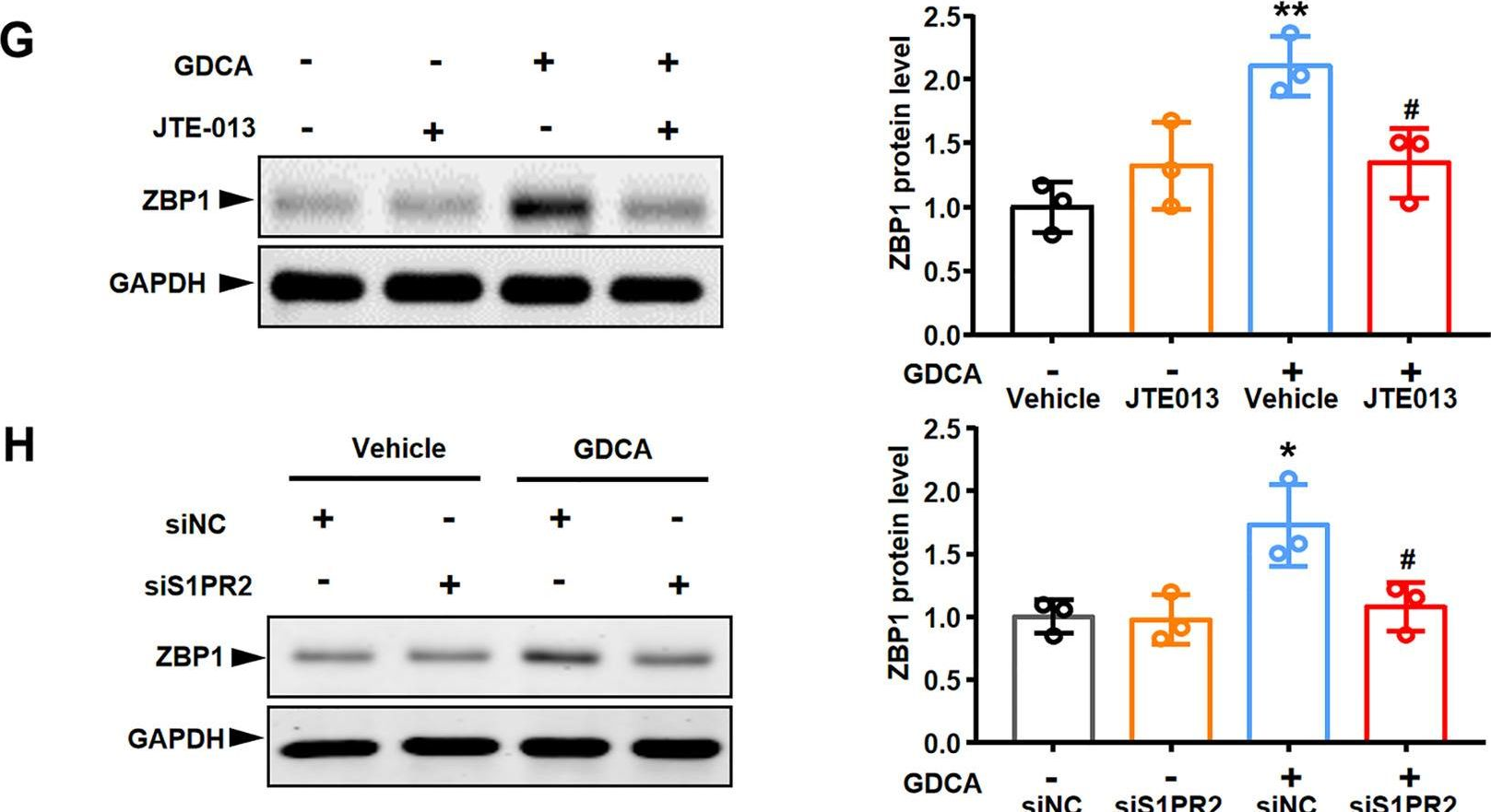
-
WB
-
Collected and cropped from Cell Death & Disease by CiteAb, provided under a CC-BY license
Image 1 of 6
In Front Cell Infect Microbiol on 8 November 2022 by Liu, J. X., Liu, M., et al.
Fig.5.C

-
WB
-
Collected and cropped from Frontiers in Cellular and Infection Microbiology by CiteAb, provided under a CC-BY license
Image 1 of 6
In Front Cell Infect Microbiol on 8 November 2022 by Liu, J. X., Liu, M., et al.
Fig.8.F
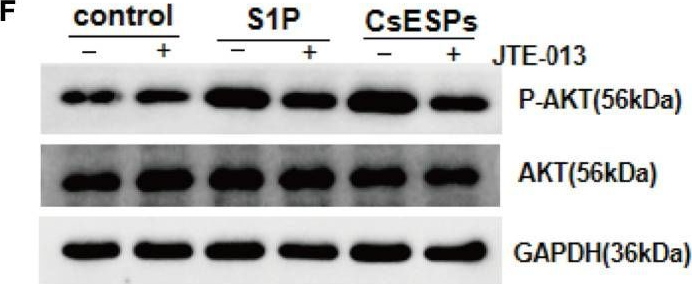
-
WB
-
Collected and cropped from Frontiers in Cellular and Infection Microbiology by CiteAb, provided under a CC-BY license
Image 1 of 6
In Front Cell Infect Microbiol on 8 November 2022 by Liu, J. X., Liu, M., et al.
Fig.6.C
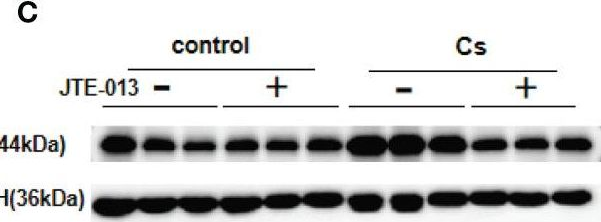
-
WB
-
Collected and cropped from Frontiers in Cellular and Infection Microbiology by CiteAb, provided under a CC-BY license
Image 1 of 6
