Pancreatic ductal adenocarcinoma (PDAC) is a highly aggressive cancer characterised by poor survival rates and an increasing global incidence. Advances in the staging and categorization of pancreatic tumours, along with the discovery of functional mutations, have made precision treatments possible, which may lead to better clinical results. To further improve customized treatment approaches, in vitro models that can be used for functional drug sensitivity testing and precisely mimic the disease at the organ level are required. In this study, we present a workflow for creating a personalized PDAC chip utilising primary tumour-derived human pancreatic organoids (hPOs) and Human Umbilical Vein Endothelial Cells (HUVECs) to simulate the vascular barrier and tumour interactions within a PDMS-free organ-on-a-chip system. The patient PDAC tissue, expanded as tumour hPOs, could be cultured as adherent cells on the chip for more than 50 days, allowing continuous monitoring of cell viability through outflows from tumour and endothelial channels. Our findings demonstrate a gradual increase in cell density and cell turnover in the pancreatic tumor channel. Tumour-specific biomarkers, including CA-19.9, TIMP-1, Osteopontin, MIC-1, ICAM-1 and sAXL were consistently detected in the PDAC chip outflows. Comparative analyses between tissue culture plates and microfluidic conditions revealed significant differences in biomarker secretion patterns, highlighting the advantages of the microfluidics approach. This PDAC chip provides a stable, reproducible tumour model system with a functional endothelial cell barrier, suitable for drug sensitivity and secretory biomarker studies, thus serving as a platform for functional precision medicine application and multi-organ chip development.
© 2024 The Authors.
Product Citations: 33
In Materials Today. Bio on 1 December 2024 by Goluba, K., Parfejevs, V., et al.
-
FC/FACS
-
Homo sapiens (Human)
-
Cancer Research
Nucleolar protein TAAP1/C22orf46 confers pro-survival signaling in non-small cell lung cancer.
In Life Science Alliance on 1 April 2024 by Döring, M., Brux, M., et al.
Tumor cells subvert immune surveillance or lytic stress by harnessing inhibitory signals. Hence, bispecific antibodies have been developed to direct CTLs to the tumor site and foster immune-dependent cytotoxicity. Although applied with success, T cell-based immunotherapies are not universally effective partially because of the expression of pro-survival factors by tumor cells protecting them from apoptosis. Here, we report a CRISPR/Cas9 screen in human non-small cell lung cancer cells designed to identify genes that confer tumors with the ability to evade the cytotoxic effects of CD8+ T lymphocytes engaged by bispecific antibodies. We show that the gene C22orf46 facilitates pro-survival signals and that tumor cells devoid of C22orf46 expression exhibit increased susceptibility to T cell-induced apoptosis and stress by genotoxic agents. Although annotated as a non-coding gene, we demonstrate that C22orf46 encodes a nucleolar protein, hereafter referred to as "Tumor Apoptosis Associated Protein 1," up-regulated in lung cancer, which displays remote homologies to the BH domain containing Bcl-2 family of apoptosis regulators. Collectively, the findings establish TAAP1/C22orf46 as a pro-survival oncogene with implications to therapy.
© 2024 Döring et al.
-
Cancer Research
EZH2 Inhibition Promotes Tumor Immunogenicity in Lung Squamous Cell Carcinomas.
In Cancer Res Commun on 13 February 2024 by DuCote, T. J., Song, X., et al.
Two important factors that contribute to resistance to immune checkpoint inhibitors (ICI) are an immune-suppressive microenvironment and limited antigen presentation by tumor cells. In this study, we examine whether inhibition of the methyltransferase enhancer of zeste 2 (EZH2) can increase ICI response in lung squamous cell carcinomas (LSCC). Our in vitro experiments using two-dimensional human cancer cell lines as well as three-dimensional murine and patient-derived organoids treated with two inhibitors of the EZH2 plus IFNγ showed that EZH2 inhibition leads to expression of both MHC class I and II (MHCI/II) expression at both the mRNA and protein levels. Chromatin immunoprecipitation sequencing confirmed loss of EZH2-mediated histone marks and gain of activating histone marks at key loci. Furthermore, we demonstrate strong tumor control in models of both autochthonous and syngeneic LSCC treated with anti-PD1 immunotherapy with EZH2 inhibition. Single-cell RNA sequencing and immune cell profiling demonstrated phenotypic changes toward more tumor suppressive phenotypes in EZH2 inhibitor-treated tumors. These results indicate that EZH2 inhibitors could increase ICI responses in patients undergoing treatment for LSCC.
The data described here show that inhibition of the epigenetic enzyme EZH2 allows derepression of multiple immunogenicity factors in LSCC, and that EZH2 inhibition alters myeloid cells in vivo. These data support clinical translation of this combination therapy for treatment of this deadly tumor type.
© 2024 The Authors; Published by the American Association for Cancer Research.
-
Cancer Research
-
Immunology and Microbiology
EZH2 inhibition promotes tumor immunogenicity in lung squamous cell carcinomas
Preprint on BioRxiv : the Preprint Server for Biology on 8 June 2023 by DuCote, T. J., Song, X., et al.
ABSTRACT Two important factors that contribute to resistance to immune checkpoint inhibitors (ICIs) are an immune-suppressive microenvironment and limited antigen presentation by tumor cells. In this study, we examine if inhibition of the methyltransferase EZH2 can increase ICI response in lung squamous cell carcinomas (LSCCs). Our in vitro experiments using 2D human cancer cell lines as well as 3D murine and patient derived organoids treated with two inhibitors of the EZH2 plus interferon-γ (IFNγ) showed that EZH2 inhibition leads to expression of both major histocompatibility complex class I and II (MHCI/II) expression at both the mRNA and protein levels. ChIP-sequencing confirmed loss of EZH2-mediated histone marks and gain of activating histone marks at key loci. Further, we demonstrate strong tumor control in models of both autochthonous and syngeneic LSCC treated with anti-PD1 immunotherapy with EZH2 inhibition. Single-cell RNA sequencing and immune cell profiling demonstrated phenotypic changes towards more tumor suppressive phenotypes in EZH2 inhibitor treated tumors. These results indicate that this therapeutic modality could increase ICI responses in patients undergoing treatment for LSCC.
-
Cancer Research
-
Immunology and Microbiology
Preprint on BioRxiv : the Preprint Server for Biology on 12 April 2023 by Schuster, E., Dashzeveg, N., et al.
Metastasis is the cause of over 90% of all deaths associated with breast cancer, yet the strategies to predict cancer spreading based on primary tumor profiles and therefore prevent metastasis are egregiously limited. As rare precursor cells to metastasis, circulating tumor cells (CTCs) in multicellular clusters in the blood are 20-50 times more likely to produce viable metastasis than single CTCs. However, the molecular mechanisms underlying various CTC clusters, such as homotypic tumor cell clusters and heterotypic tumor-immune cell clusters, are yet to be fully elucidated. Combining machine learning-assisted computational ranking with experimental demonstration to assess cell adhesion candidates, we identified a transmembrane protein Plexin- B2 (PB2) as a new therapeutic target that drives the formation of both homotypic and heterotypic CTC clusters. High PB2 expression in human primary tumors predicts an unfavorable distant metastasis-free survival and is enriched in CTC clusters compared to single CTCs in advanced breast cancers. Loss of PB2 reduces formation of homotypic tumor cell clusters as well as heterotypic tumor-myeloid cell clusters in triple-negative breast cancer. Interactions between PB2 and its ligand Sema4C on tumor cells promote homotypic cluster formation, and PB2 binding with Sema4A on myeloid cells (monocytes) drives heterotypic CTC cluster formation, suggesting that metastasizing tumor cells hijack the PB2/Sema family axis to promote lung metastasis in breast cancer. Additionally, using a global proteomic analysis, we identified novel downstream effectors of the PB2 pathway associated with cancer stemness, cell cycling, and tumor cell clustering in breast cancer. Thus, PB2 is a novel therapeutic target for preventing new metastasis.
-
Cancer Research
In Cell Oncol (Dordr) on 1 December 2018 by Sun, X., Martin, R. C. G., et al.
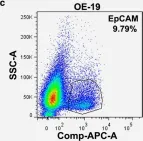
Fig.1.C

-
FC/FACS
-
Collected and cropped from Cell Oncol (Dordr) by CiteAb, provided under a CC-BY license
Image 1 of 1