Lentiviral vector (LV)-mediated ex vivo gene therapy for haematopoietic stem and progenitor cells (HSPCs) has delivered on the promise of a 'one-and-done' treatment for several genetic diseases1. However, ex vivo manipulation and patient conditioning before transplantation are major hurdles that could be overcome by an in vivo approach. Here we demonstrate that in vivo gene delivery to HSPCs after systemic LV administration is enabled by the substantial trafficking of these cells from the liver to the bone marrow in newborn mice. We improved gene-transfer efficiency using a phagocytosis-shielded LV, successfully reaching bona fide HSPCs capable of long-term multilineage output and engraftment after serial transplantation, as confirmed by clonal tracking. HSPC mobilization further increased gene transfer, extending the window of intervention, although permissiveness to LV transduction declined with age. We successfully tested this in vivo strategy in mouse models of adenosine deaminase deficiency, autosomal recessive osteopetrosis and Fanconi anaemia. Interestingly, in vivo gene transfer provided a selective advantage to corrected HSPCs in Fanconi anaemia, leading to near-complete haematopoietic reconstitution and prevention of bone marrow failure. Given that circulating HSPCs in humans are also most abundant shortly after birth, in vivo HSPC gene transfer holds strong translational potential across multiple diseases.
© 2025. The Author(s).
Product Citations: 172
In vivo haemopoietic stem cell gene therapy enabled by postnatal trafficking.
In Nature on 28 May 2025 by Milani, M., Fabiano, A., et al.
-
Stem Cells and Developmental Biology
In Alzheimer's Dementia : the Journal of the Alzheimer's Association on 1 February 2025 by Yu, Z. Y., Liu, J., et al.
The triggering receptor expressed on myeloid cells 2 (TREM2) arginine-47-histidine (R47H) mutation is a significant risk for Alzheimer's disease (AD) with unclear mechanisms. Previous studies focused on microglial amyloid-β (Aβ) phagocytosis with less attention on the impact of TREM2R47H mutation on blood monocytes.
Bone marrow transplantation (BMT) models were used to assess the contribution of blood monocytes carrying TREM2R47H mutation to AD.
Aβ phagocytosis was compromised in mouse monocytes carrying the TREM2R47H mutation. Transplantation of bone marrow cells (BMCs) carrying TREM2R47H mutation increased cerebral Aβ burden and aggravated AD-type pathologies. Moreover, the replacement of TREM2R47H-BMCs restored monocytic Aβ phagocytosis, lowered Aβ levels in the blood and brain, and improved cognitive function.
Our study reveals that blood monocytes carrying the TREM2R47H mutation substantially contribute to the pathogenesis of AD, and correcting the TREM2R47H mutation in BMCs would be a potential therapeutic approach for those carrying this mutation.
TREM2R47H mutation compromises the Aβ phagocytosis of blood monocytes. Blood monocytes carrying TREM2R47H mutation contribute substantially to AD pathogenesis. Correction of the TREM2R47H mutation in bone marrow cells ameliorates AD pathologies and cognitive impairments.
© 2025 The Author(s). Alzheimer's & Dementia published by Wiley Periodicals LLC on behalf of Alzheimer's Association.
-
Cardiovascular biology
-
Neuroscience
Safety Evaluations of Rapamycin Perfluorocarbon Nanoparticles in Ovarian Tumor-Bearing Mice.
In Nanomaterials (Basel, Switzerland) on 31 October 2024 by Zhou, Q., Harding, J. C., et al.
Nanomedicine holds great potential for revolutionizing medical treatment. Ongoing research and advancements in nanotechnology are continuously expanding the possibilities, promising significant advancements in healthcare. To fully harness the potential of nanotechnology in medical applications, it is crucial to conduct safety evaluations for the nanomedicines that offer effective benefits in the preclinical stage. Our recent efficacy studies indicated that rapamycin perfluorocarbon (PFC) nanoparticles showed promise in mitigating cisplatin-induced acute kidney injury (AKI). As cisplatin is routinely administered to ovarian cancer patients as their first-line chemotherapy, in this study, we focused on evaluating the safety of rapamycin PFC nanoparticles in mice bearing ovarian tumor xenografts. Specifically, this study evaluated the effects of repeat-dose rapamycin PFC nanoparticle treatment on vital organs, the immune system, and tumor growth and assessed pharmacokinetics and biodistribution. Our results indicated that rapamycin PFC nanoparticle treatment did not cause any detectable adverse effects on cardiac, renal, or hepatic functions or on splenocyte populations, but it reduced the splenocyte secretion of IL-10, TNFα, and IL12p70 upon IgM stimulation. The pharmacokinetics and biodistribution results revealed a significant enhancement in the delivery of rapamycin to tumors by rapamycin PFC nanoparticles, which, in turn, led to a significant reduction in ovarian tumor growth. Therefore, rapamycin PFC nanoparticles have the potential to be clinically beneficial in cisplatin-treated ovarian cancer patients.
-
Mus musculus (House mouse)
-
Cancer Research
In Journal for Immunotherapy of Cancer on 5 September 2024 by Mei, D., Xue, Z., et al.
In allogeneic-hematopoietic stem cell transplantation for acute myeloid leukemia (AML), donor T cells combat leukemia through the graft-versus-leukemia (GVL) effect, while they also pose a risk of triggering life-threatening graft-versus-host disease (GVHD) by interacting with recipient cells. The onset of GVHD hinges on the interplay between donor T cells and recipient antigen-presenting cells (APCs), sparking T-cell activation. However, effective methods to balance GVHD and GVL are lacking.
In our study, we crafted nanocapsules by layering polycationic aminated gelatin and polyanionic alginate onto the surface of T cells, examining potential alterations in their fundamental physiological functions. Subsequently, we established an AML mouse model and treated it with transplantation of bone marrow cells (BMCs) combined with encapsulated T cells to investigate the GVL and anti-GVHD effects of encapsulated T cells. In vitro co-culture was employed to probe the effects of encapsulation on immune synapses, co-stimulatory molecules, and tumor-killing pathways.
Transplantation of BMCs combined with donor T cells selectively encapsulated onto AML mice significantly alleviates GVHD symptoms while preserving essential GVL effects. Encapsulated T cells exerted their immunomodulatory effects by impeding the formation of immune synapses with recipient APCs, thereby downregulating co-stimulatory signals such as CD28-CD80, ICOS-ICOSL, and CD40L-CD40. Recipient mice receiving encapsulated T-cell transplantation exhibited a marked increase in donor Ly-5.1-BMC cell numbers, accompanied by unaltered in vivo expression levels of perforin and granzyme B. While transient inhibition of donor T-cell cytotoxicity in the tumor microenvironment was observed in vitro following single-cell nanoencapsulation, subsequent restoration to normal antitumor activity ensued, attributed to selective permeability of encapsulated vesicle shells and material degradation. Moreover, the expression of apoptotic proteins and FAS-FAS ligand pathway at normal levels was still observed in leukemia tumor cells.
Encapsulated donor T cells effectively mitigate GVHD while preserving the GVL effect by minimizing co-stimulatory signaling with APCs through early immune isolation. Subsequent degradation of nanocapsules restores T-cell cytotoxic efficacy against AML cells, mediated by cytotoxic pathways. Using transplant-encapsulated T cells offers a promising strategy to suppress GVHD while preserving the GVL effect.
© Author(s) (or their employer(s)) 2024. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
-
Immunology and Microbiology
In International Journal of Biological Sciences on 21 June 2024 by Zhang, X., Zhang, Z., et al.
Rheumatoid arthritis (RA) is a chronic systemic autoimmune disease characterized by synovial inflammation and the production of autoantibodies. Previous studies have indicated an association between high-salt diets (HSD) and an increased risk of RA, yet the underlying mechanisms remain unclear. Macrophage pyroptosis, a pro-inflammatory form of cell death, plays a pivotal role in RA. In this study, we demonstrate that HSD exacerbates the severity of arthritis in collagen-induced arthritis (CIA) mice, correlating with macrophage infiltration and inflammatory lesions. Given the significant alterations observed in macrophages from CIA mice subjected to HSD, we specifically investigate the impact of HSD on macrophage responses in the inflammatory milieu of RA. In our in vitro experiments, pretreatment with NaCl enhances LPS-induced pyroptosis in RAW.264.7 and THP-1 cells through the p38 MAPK/NF-κB signaling pathway. Subsequent experiments reveal that Slc6a12 inhibitors and SGK1 silencing inhibit sodium-induced activation of macrophage pyroptosis and the p38 MAPK/NF-κB signaling pathway, whereas overexpression of the SGK1 gene counteracts the effect of sodium on macrophages. In conclusion, our findings verified that high salt intake promotes the progression of RA and provided a detailed elucidation of the activation of macrophage pyroptosis induced by sodium transportation through the Slc6a12 channel.
© The author(s).
-
FC/FACS
-
Mus musculus (House mouse)
-
Immunology and Microbiology
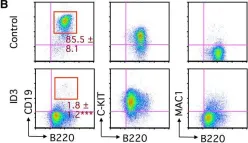
In Stem Cell Reports on 10 November 2015 by Ikawa, T., Masuda, K., et al.
Fig.1.B

-
FC/FACS
-
Mus musculus (House mouse)
Collected and cropped from Stem Cell Reports by CiteAb, provided under a CC-BY license
Image 1 of 1