We previously established a feeder-free cell therapy platform for the ex vivo generation of lymphoid-primed progenitors using immobilized Delta-like ligand 4 (DLL4). In vivo studies demonstrated that adoptive transfer of these progenitors accelerates T cell reconstitution following thymic engraftment.
To further explore the full therapeutic potential of this cell product, we performed a comprehensive molecular and phenotypic characterization using single cell RNA sequencing and mass cytometry analysis.
Our analysis revealed the presence of distinct cell subsets within the cellular product characterized mainly by commitment to lymphoid lineages. Using integrated transcriptomic analyses to compare these ex vivo-generated progenitors to in vivo human thymocytes, we revealed strong similarities with early stages of T cell development, underscoring the physiological relevance of our system. We also delineated two distinct developmental trajectories within the CD7+ progenitor population: a T cell-oriented path, marked by CD5 upregulation, and an innate lymphoid cell (ILC)-oriented branch, identified by CD161 expression and an ILC-like gene signature. Despite these lineage predispositions, both subsets demonstrated plasticity, retaining the ability to differentiate into both T cells and natural killer (NK) cells in vitro. Additionally, in our experimental setting, we observed that BCL11B, a transcription factor essential for T cell commitment, regulates negatively myeloid cell differentiation while preserving the potential for NK cell development.
These findings underscore the versatility of DLL4-based lymphoid progenitors in generating either T cells or ILCs in response to environmental cues. This research paves the way for innovative cell therapy approaches to treat immune deficiencies and cancer- and age-related immune dysfunctions.
Copyright © 2025 Gaudeaux, Paillet, Abou Alezz, Moirangthem, Cascione, Martin Corredera, Dolens, De Mulder, Velghe, Vandekerckhove, Lavaert, Robil, Corneau, Sadek, Rault, Joshi, de la Grange, Staal, Taghon, Negre, Ditadi, André and Soheili.
Product Citations: 103
Ex vivo-generated lymphoid progenitors encompass both T cell and innate lymphoid cell fates.
In Frontiers in Immunology on 7 August 2025 by Gaudeaux, P., Paillet, J., et al.
-
Immunology and Microbiology
Microbial metabolite drives ageing-related clonal haematopoiesis via ALPK1.
In Nature on 1 June 2025 by Agarwal, P., Sampson, A. M., et al.
Clonal haematopoiesis of indeterminate potential (CHIP) involves the gradual expansion of mutant pre-leukaemic haematopoietic cells, which increases with age and confers a risk for multiple diseases, including leukaemia and immune-related conditions1. Although the absolute risk of leukaemic transformation in individuals with CHIP is very low, the strongest predictor of progression is the accumulation of mutant haematopoietic cells2. Despite the known associations between CHIP and increased all-cause mortality, our understanding of environmental and regulatory factors that underlie this process during ageing remains rudimentary. Here we show that intestinal alterations, which can occur with age, lead to systemic dissemination of a microbial metabolite that promotes pre-leukaemic cell expansion. Specifically, ADP-D-glycero-β-D-manno-heptose (ADP-heptose), a biosynthetic bi-product specific to Gram-negative bacteria3-5, is uniquely found in the circulation of older individuals and favours the expansion of pre-leukaemic cells. ADP-heptose is also associated with increased inflammation and cardiovascular risk in CHIP. Mechanistically, ADP-heptose binds to its receptor, ALPK1, triggering transcriptional reprogramming and NF-κB activation that endows pre-leukaemic cells with a competitive advantage due to excessive clonal proliferation. Collectively, we identify that the accumulation of ADP-heptose represents a direct link between ageing and expansion of rare pre-leukaemic cells, suggesting that the ADP-heptose-ALPK1 axis is a promising therapeutic target to prevent progression of CHIP to overt leukaemia and immune-related conditions.
© 2025. The Author(s).
-
Cell Biology
In Nature Communications on 1 April 2025 by Feist, W. N., Luna, S. E., et al.
Allogeneic transplantation of CCR5 null hematopoietic stem and progenitor cells (HSPCs) is the only known cure for HIV-1 infection. However, this treatment is limited because of the rarity of CCR5-null matched donors, the morbidities associated with allogeneic transplantation, and the prevalence of HIV-1 strains resistant to CCR5 knockout (KO) alone. Here, we propose a one-time therapy through autologous transplantation of HSPCs genetically engineered ex vivo to produce both CCR5 KO cells and long-term secretion of potent HIV-1 inhibiting antibodies from B cell progeny. CRISPR-Cas9-engineered HSPCs engraft and reconstitute multiple hematopoietic lineages in vivo and can be engineered to express multiple antibodies simultaneously (in pre-clinical models). Human B cells engineered to express each antibody secrete neutralizing concentrations capable of inhibiting HIV-1 pseudovirus infection in vitro. This work lays the foundation for a potential one-time functional cure for HIV-1 through combining the long-term delivery of therapeutic antibodies against HIV-1 and the known efficacy of CCR5 KO HSPC transplantation.
© 2025. The Author(s).
-
Immunology and Microbiology
S100A9 and HMGB1 orchestrate MDSC-mediated immunosuppression in melanoma through TLR4 signaling.
In Journal for Immunotherapy of Cancer on 11 September 2024 by Ozbay Kurt, F. G., Cicortas, B. A., et al.
Immunotherapies for malignant melanoma are challenged by the resistance developed in a significant proportion of patients. Myeloid-derived suppressor cells (MDSC), with their ability to inhibit antitumor T-cell responses, are a major contributor to immunosuppression and resistance to immune checkpoint therapies in melanoma. Damage-associated molecular patterns S100A8, S100A9, and HMGB1, acting as toll like receptor 4 (TLR4) and receptor for advanced glycation endproducts (RAGE) ligands, are highly expressed in the tumor microenvironment and drive MDSC activation. However, the role of TLR4 and RAGE signaling in the acquisition of MDSC immunosuppressive properties remains to be better defined. Our study investigates how the signaling via TLR4 and RAGE as well as their ligands S100A9 and HMGB1, shape MDSC-mediated immunosuppression in melanoma.
MDSC were isolated from the peripheral blood of patients with advanced melanoma or generated in vitro from healthy donor-derived monocytes. Monocytes were treated with S100A9 or HMGB1 for 72 hours. The immunosuppressive capacity of treated monocytes was assessed in the inhibition of T-cell proliferation assay in the presence or absence of TLR4 and RAGE inhibitors. Plasma levels of S100A8/9 and HMGB1 were quantified by ELISA. Single-cell RNA sequencing (scRNA-seq) was performed on monocytes from patients with melanoma and healthy donors.
We showed that exposure to S100A9 and HMGB1 converted healthy donor-derived monocytes into MDSC through TLR4 signaling. Our scRNA-seq data revealed in patient monocytes enriched inflammatory genes, including S100 and those involved in NF-κB and TLR4 signaling, and a reduced major histocompatibility complex II gene expression. Furthermore, elevated plasma S100A8/9 levels correlated with shorter progression-free survival in patients with melanoma.
These findings highlight the critical role of TLR4 and, to a lesser extent, RAGE signaling in the conversion of monocytes into MDSC-like cells, underscore the potential of targeting S100A9 to prevent this conversion, and highlight the prognostic value of S100A8/9 as a plasma biomarker in melanoma.
© Author(s) (or their employer(s)) 2024. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
-
Homo sapiens (Human)
-
Cancer Research
In NPJ Vaccines on 26 June 2024 by Edwards, K. R., Malhi, H., et al.
Epstein-Barr virus (EBV) is associated with several malignancies, neurodegenerative disorders and is the causative agent of infectious mononucleosis. A vaccine that prevents EBV-driven morbidity and mortality remains an unmet need. EBV is orally transmitted, infecting both B cells and epithelial cells. Several virally encoded proteins are involved in entry. The gH/gL glycoprotein complex is essential for infectivity irrespective of cell type, while gp42 is essential for infection of B cells. gp350 promotes viral attachment by binding to CD21 or CD35 and is the most abundant glycoprotein on the virion. gH/gL, gp42 and gp350, are known targets of neutralizing antibodies and therefore relevant immunogens for vaccine development. Here, we developed and optimized the delivery of several alphavirus-derived replicon RNA (repRNA) vaccine candidates encoding gH/gL, gH/gL/gp42 or gp350 delivered by a cationic nanocarrier termed LION™. The lead candidate, encoding full-length gH/gL, elicited high titers of neutralizing antibodies that persisted for at least 8 months and a vaccine-specific CD8+ T cell response. Transfer of vaccine-elicited IgG protected humanized mice from EBV-driven tumor formation and death following high-dose viral challenge. These data demonstrate that LION/repRNA-gH/gL is an ideal candidate vaccine for preventing EBV infection and/or related malignancies in humans.
© 2024. The Author(s).
-
Immunology and Microbiology
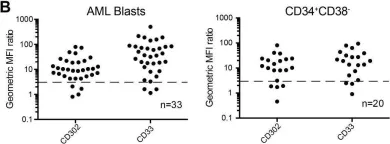
In PLoS One on 11 May 2019 by Lo, T. H., Abadir, E., et al.
Fig.1.B

-
FC/FACS
-
Collected and cropped from PLoS One by CiteAb, provided under a CC-BY license
Image 1 of 1