Immunogenicity refers to the ability of a substance, such as a therapeutic drug, to elicit an immune response. While beneficial in vaccine development, undesirable immunogenicity can compromise the safety and efficacy of therapeutic proteins by inducing anti-drug antibodies (ADAs). These ADAs can reduce drug bioavailability and alter pharmacokinetics, necessitating comprehensive immunogenicity risk assessments starting at early stages of drug development. Given the complexity of immunogenicity, an integrated approach is essential, as no single assay can universally recapitulate the immune response leading to the formation of anti-drug antibodies.
To better understand the Dendritic Cell (DC) contribution to immunogenicity, we developed two flow cytometry-based assays: the DC internalization assay and the DC activation assay. Monocyte-derived dendritic cells (moDCs) were generated from peripheral blood mononuclear cells (PBMCs) and differentiated over a five-day period. The internalization assay measured the accumulation rate of therapeutic antibodies within moDCs, while the activation assay assessed the expression of DC activation markers such as CD40, CD80, CD86, CD83, and DC-SIGN (CD209). To characterize these two assays further, we used a set of marketed therapeutic antibodies.
The study highlights that moDCs differentiated for 5 days from freshly isolated monocytes were more prone to respond to external stimuli. The internalization assay has been shown to be highly sensitive to the molecule tested, allowing the use of only 4 donors to detect small but significant differences. We also demonstrated that therapeutic antibodies were efficiently taken up by moDCs, with a strong correlation with their peptide presentation on MHC-II. On the other hand, by monitoring DC activation through a limited set of activation markers including CD40, CD83, and DC-SIGN, the DC activation assay has the potential to compare a series of compounds. These two assays provide a more comprehensive understanding of DC function in the context of immunogenicity, highlighting the importance of both internalization and activation processes in ADA development.
The DC internalization and activation assays described here address key gaps in existing immunogenicity assessment methods by providing specific and reliable measures of DC function. The assays enhance our ability to pre-clinically evaluate the immunogenic potential of biotherapeutics, thereby improving their safety and efficacy. Future work should focus on further validating these assays and integrating them into a holistic immunogenicity risk assessment framework.
Copyright © 2024 Siegel, Padamsey, Bolender, Hargreaves, Fraidling, Ducret, Hartman, Looney, Bertinetti-Lapatki, Rohr, Hickling, Kraft and Marban-Doran.
Product Citations: 94
In Frontiers in Immunology on 4 September 2024 by Siegel, M., Padamsey, A., et al.
-
FC/FACS
-
Homo sapiens (Human)
-
Immunology and Microbiology
In Journal of Cellular and Molecular Medicine on 1 September 2024 by Torabi, S., Zarrabi, M., et al.
The potential of extracellular vesicles (EVs) isolated from mesenchymal stromal cells in guiding macrophages toward anti-inflammatory immunophenotypes, has been reported in several studies. In our study, we provided experimental evidence of a distinctive effect played by Wharton Jelly mesenchymal stromal cell-derived EVs (WJ-EVs) on human macrophages. We particularly analyzed their anti-inflammatory effects on macrophages by evaluating their interactions with stellate cells, and their protective role in liver fibrosis. A three-step gradient method was used to isolate monocytes from umbilical cord blood (UCB). Two subpopulations of WJ-EVs were isolated by high-speed (20,000 g) and differential ultracentrifugation (110,000 g). Further to their characterization, they were designated as EV20K and EV110K and incubated at different concentrations with UCB-derived monocytes for 7 days. Their anti-fibrotic effect was assessed by studying the differentiation and functional levels of generated macrophages and their potential to modulate the survival and activity of LX2 stellate cells. The EV20K triggers the polarization of UCB-derived monocytes towards a peculiar M2-like functional phenotype more effectively than the M-CSF positive control. The EV20K treated macrophages were characterized by a higher expression of scavenger receptors, increased phagocytic capacity and production level of interleukin-10 and transforming growth factor-β. Conditioned medium from those polarized macrophages attenuated the proliferation, contractility and activation of LX2 stellate cells. Our data show that EV20K derived from WJ-MSCs induces activated macrophages to suppress immune responses and potentially play a protective role in the pathogenesis of liver fibrosis by directly inhibiting HSC's activation.
© 2024 The Author(s). Journal of Cellular and Molecular Medicine published by Foundation for Cellular and Molecular Medicine and John Wiley & Sons Ltd.
-
Biochemistry and Molecular biology
-
Stem Cells and Developmental Biology
In Biomedicines on 20 August 2024 by Gagliardi, M., Kean, R., et al.
Overexpression and aberrant activation of signal transducer and activator of transcription 3 (STAT3) contribute to tumorigenesis, drug resistance, and tumor-immune evasion, making it a potential cancer therapeutic target. BP1003 is a neutral liposome incorporated with a nuclease-resistant P-ethoxy antisense oligodeoxynucleotide (ASO) targeting the STAT3 mRNA. Its unique design enhances BP1003 stability, cellular uptake, and target affinity. BP1003 efficiently reduces STAT3 expression and enhances the sensitivity of breast cancer cells (HER2+, triple negative) and ovarian cancer cells (late stage, invasive ovarian cancer) to paclitaxel and 5-fluorouracil (5-FU) in both 2D and 3D cell cultures. Similarly, ex vivo and in vivo patient-derived models of pancreatic ductal adenocarcinoma (PDAC) show reduced tissue viability and tumor volume with BP1003 and gemcitabine combination treatments. In addition to directly affecting tumor cells, BP1003 can modulate the tumor microenvironment. Unlike M1 differentiation, monocyte differentiation into anti-inflammatory M2 macrophages is suppressed by BP1003, indicating its potential contribution to immunotherapy. The broad anti-tumor effect of BP1003 in numerous preclinical solid tumor models, such as breast, ovarian, and pancreatic cancer models shown in this work, makes it a promising cancer therapeutic.
-
Cancer Research
In Cells on 17 August 2024 by Dayoub, A. S., Acharya, E., et al.
Retinopathy of prematurity (ROP) has a dual-phase disease pathology; in phase 1, hyperoxia-induced vaso-obliteration occurs in the retinal vasculature due to increased oxidative stress (OS) and inflammation, followed by phase 2, where hypoxia increases the overproduction of growth factors, inducing retinal neovascularization. Toll-like receptor 2 and -4 (TLR2 and TLR4) overactivation, hyper-inflammation, macrophages, and neutrophil infiltration contribute to the developing ROP. AVR-121 and AVR-123 are novel classes of small-molecule dual inhibitors of TLR2/4 tested in a human leukemia monocytic cell line (THP-1) and cord-blood-derived mononuclear cells (CBMCs). Both compounds inhibited TLR2/4 signaling-related inflammatory cytokines in THP-1 cells and inhibited VEGF-induced neovascularization in human retinal endothelial cells (HRECs), which are hallmarks of ROP. In an oxygen-induced retinopathy (OIR) murine model, the intraperitoneal injection of AVR-123 in the hyperoxia phase (P7-P12) or a nanosuspension eyedrop of AVR-123 in the hypoxic phase (P12-P17) significantly reduced vaso-obliteration, angiogenesis, and inflammatory cytokine profiles while not inhibiting the necessary growth factor VEGF in the juvenile mouse eyes. The results are consistent with our hypothesis that targeting the dual TLR2/4 pathway will reduce inflammation, angiogenesis, and vaso-obliteration in vitro and in vivo and reduce cytotoxic immune cells. AVR-123 has the potential to be developed as a therapy for ROP.
-
Cell Biology
-
Immunology and Microbiology
In IScience on 16 August 2024 by Benhamouda, N., Besbes, A., et al.
Coordinating immune responses - humoral and cellular - is vital for protection against severe Covid-19. Our study evaluates a multicytokine CD4+T cell signature's predictive for post-vaccinal serological and CD8+T cell responses. A cytokine signature composed of four cytokines (IL-2, TNF-α, IP10, IL-9) excluding IFN-γ, and generated through machine learning, effectively predicted the CD8+T cell response following mRNA-1273 or BNT162b2 vaccine administration. Its applicability extends to murine vaccination models, encompassing diverse immunization routes (such as intranasal) and vaccine platforms (including adjuvanted proteins). Notably, we found correlation between CD4+T lymphocyte-produced IL-21 and the humoral response. Consequently, we propose a test that offers a rapid overview of integrated immune responses. This approach holds particular relevance for scenarios involving immunocompromised patients because they often have low cell counts (lymphopenia) or pandemics. This study also underscores the pivotal role of CD4+T cells during a vaccine response and highlights their value in vaccine immunomonitoring.
© 2024 The Authors.
-
COVID-19
-
Genetics
-
Immunology and Microbiology
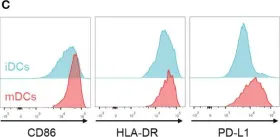
In Front Immunol on 11 February 2023 by Subtil, B., Iyer, K. K., et al.
Fig.4.C

-
FC/FACS
-
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 7
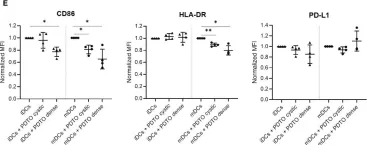
In Front Immunol on 11 February 2023 by Subtil, B., Iyer, K. K., et al.
Fig.4.E

-
FC/FACS
-
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 7
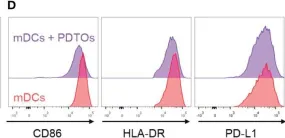
In Front Immunol on 11 February 2023 by Subtil, B., Iyer, K. K., et al.
Fig.4.D

-
FC/FACS
-
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 7
In Nat Commun on 30 April 2019 by Jardine, L., Wiscombe, S., et al.
Fig.3.A

-
FC/FACS
-
Homo sapiens (Human)
Collected and cropped from Nat Commun by CiteAb, provided under a CC-BY license
Image 1 of 7
In Front Immunol on 11 July 2018 by Remes Lenicov, F., Paletta, A. L., et al.
Fig.3.A

-
FC/FACS
-
Homo sapiens (Human)
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 7
In Front Immunol on 11 July 2018 by Remes Lenicov, F., Paletta, A. L., et al.
Fig.3.B

-
FC/FACS
-
Homo sapiens (Human)
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 7
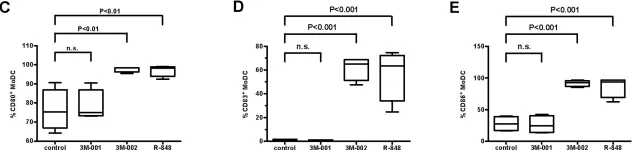
In PLoS One on 24 April 2008 by Schlaepfer, E. & Speck, R. F.
Fig.2.C,D,E
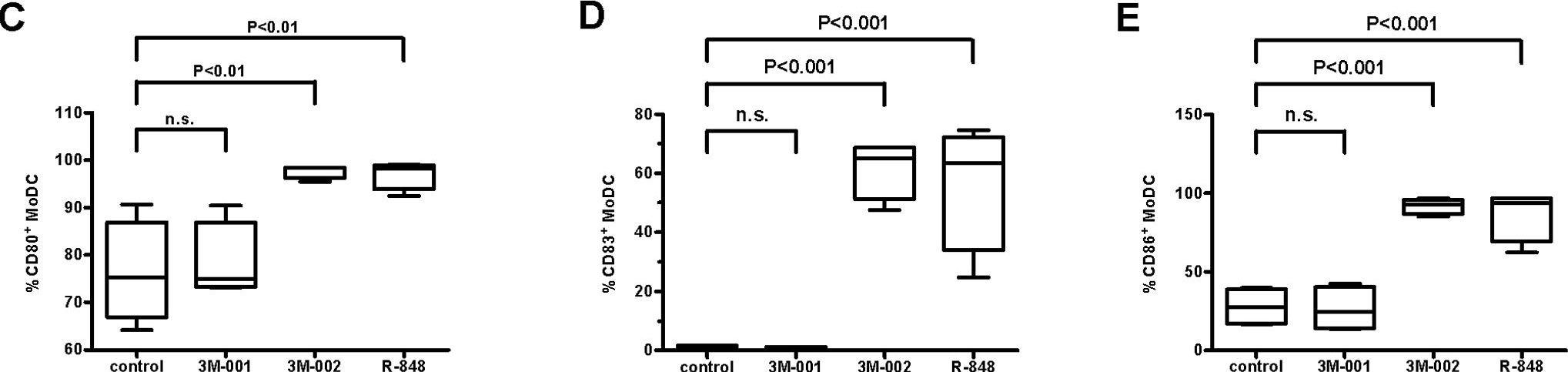
-
FC/FACS
-
Homo sapiens (Human)
Collected and cropped from PLoS One by CiteAb, provided under a CC-BY license
Image 1 of 7