PD-1 blockade therapy has revolutionized melanoma treatment, but still not all patients benefit and pre-treatment identification of those patients is difficult. Increased expression of inflammatory markers such as interleukin (IL)-6 in blood of patients correlates with poor treatment response. We set out to study the effect of inflammatory cytokines on PD-1 blockade in vitro. For this, we studied the effect of IL-6 and type I interferon (IFN) in vitro on human T cells in a mixed leukocyte reaction (MLR) in the absence or presence of PD-1 blockade. While IL-6 reduced IFN-γ secretion by T cells in both the presence and absence of PD-1 blockade, IFN-α specifically reduced the IFN-γ secretion only in the presence of PD-1 blockade. IFN-α reduced T cell proliferation independent of PD-1 blockade and reduced the percentage of cells producing IFN-γ only in the presence of PD-1 blockade. Next we determined the type I IFN score in a cohort of 22 melanoma patients treated with nivolumab. In this cohort, we did not find a correlation between clinical response and type I IFN score, nor between clinical response and IFN-γ secretion in vitro in a MLR in the presence of PD-1 blockade. We conclude that IFN-α reduces the effectiveness of PD-1 blockade in vitro, but that in this cohort, type I IFN score in vivo, nor IFN-γ secretion in vitro in a MLR in the presence of PD-1 blockade correlated to decreased therapy responses in patients.
© 2024. The Author(s).
Product Citations: 32
In Cancer Immunology, Immunotherapy : CII on 5 July 2024 by Timmerman, L. M., Hensen, L. C. M., et al.
-
Cancer Research
-
Immunology and Microbiology
In IScience on 21 June 2024 by Jansen, S. A., Cutilli, A., et al.
The intestine is vulnerable to chemotherapy-induced damage due to the high rate of intestinal epithelial cell (IEC) proliferation. We have developed a human intestinal organoid-based 3D model system to study the direct effect of chemotherapy-induced IEC damage on T cell behavior. Exposure of intestinal organoids to busulfan, fludarabine, and clofarabine induced damage-related responses affecting both the capacity to regenerate and transcriptional reprogramming. In ex vivo co-culture assays, prior intestinal organoid damage resulted in increased T cell activation, proliferation, and migration. We identified galectin-9 (Gal-9) as a key molecule released by damaged organoids. The use of anti-Gal-9 blocking antibodies or CRISPR/Cas9-mediated Gal-9 knock-out prevented intestinal organoid damage-induced T cell proliferation, interferon-gamma release, and migration. Increased levels of Gal-9 were found early after HSCT chemotherapeutic conditioning in the plasma of patients who later developed acute GVHD. Taken together, chemotherapy-induced intestinal damage can influence T cell behavior in a Gal-9-dependent manner which may provide novel strategies for therapeutic intervention.
© 2024 The Author(s).
-
Immunology and Microbiology
In The Journal of Immunology on 1 June 2024 by Vemulawada, C., Renavikar, P. S., et al.
An imbalance between proinflammatory and regulatory processes underlies autoimmune disease pathogenesis. We have shown that acute relapses of multiple sclerosis are characterized by a deficit in the immune suppressive ability of CD8+ T cells. These cells play an important immune regulatory role, mediated in part through cytotoxicity (perforin [PRF]/granzyme [GZM]) and IFNγ secretion. In this study, we further investigated the importance of IFNγ-, GZMB-, PRF1-, and LYST-associated pathways in CD8+ T cell-mediated suppression. Using the CRISPR-Cas9 ribonucleoprotein transfection system, we first optimized efficient gene knockout while maintaining high viability in primary bulk human CD8+ T cells. Knockout was confirmed through quantitative real-time PCR assays in all cases, combined with flow cytometry where appropriate, as well as confirmation of insertions and/or deletions at genomic target sites. We observed that the knockout of IFNγ, GZMB, PRF1, or LYST, but not the knockout of IL4 or IL5, resulted in significantly diminished in vitro suppressive ability in these cells. Collectively, these results reveal a pivotal role for these pathways in CD8+ T cell-mediated immune suppression and provide important insights into the biology of human CD8+ T cell-mediated suppression that could be targeted for immunotherapeutic intervention.
Copyright © 2024 by The American Association of Immunologists, Inc.
-
Immunology and Microbiology
In Nature Communications on 8 August 2023 by Dasari, V., McNeil, L. K., et al.
The recent emergence of a causal link between Epstein-Barr virus (EBV) and multiple sclerosis has generated considerable interest in the development of an effective vaccine against EBV. Here we describe a vaccine formulation based on a lymph node targeting Amphiphile vaccine adjuvant, Amphiphile-CpG, admixed with EBV gp350 glycoprotein and an engineered EBV polyepitope protein that includes 20 CD8+ T cell epitopes from EBV latent and lytic antigens. Potent gp350-specific IgG responses are induced in mice with titers >100,000 in Amphiphile-CpG vaccinated mice. Immunization including Amphiphile-CpG also induces high frequencies of polyfunctional gp350-specific CD4+ T cells and EBV-specific CD8+ T cells that are 2-fold greater than soluble CpG and are maintained for >7 months post immunization. This combination of broad humoral and cellular immunity against multiple viral determinants is likely to provide better protection against primary infection and control of latently infected B cells leading to protection against the development of EBV-associated diseases.
© 2023. The Author(s).
-
Immunology and Microbiology
In BMC Gastroenterology on 11 March 2023 by Gao, X., Duan, S., et al.
Monocytes/macrophages play important roles in inflammatory bowel disease and depression, but few studies had focused on the change of monocytes/macrophages in ulcerative colitis (UC) patients with psychiatric disorders.
UC patients were divided into two groups based on the Hospital Anxiety and Depression Scale (HADS). Demographic and clinical data were captured. Peripheral blood samples and intestinal biopsies were collected for the analysis of monocyte immunophenotype, phagocytic function, and CD4 + T cell differentiation. Transmission electron microscopy was used to observe the ultrastructure of intestinal macrophages.
A total of 139 UC patients were included. 37.41% and 32.37% of UC patients had symptoms of anxiety and depression. In patients with symptoms of anxiety/depression, mayo score, platelet count, erythrocyte sedimentation rate, and endoscopic score, histological scores were significantly higher than those in UC patients without. In patients with symptoms of anxiety/depression, the percentages of CD14 + + CD16 + monocytes and CD14 + CD16++ monocytes were higher, and the phagocytosis was decreased. Patients with symptoms of anxiety/depression had more CD68 + cells and higher M1/M2 ratios in the intestine mucosal layer compared to those without.
Monocytes and intestinal macrophages from UC patients with anxiety/depression tended to polarize to pro-inflammatory subtypes, and their function was also impaired.
© 2023. The Author(s).
-
Homo sapiens (Human)
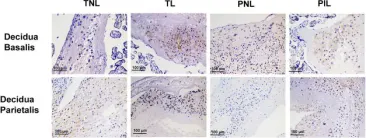
In Front Immunol on 28 June 2022 by Zha, Y., Liu, H., et al.
Fig.5.A

-
IHC-P
-
Homo sapiens (Human)
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 1