Patients with interstitial lung disease (ILD) and severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) infection are at high risk of severe coronavirus disease 2019. It is unclear whether anti-viral cellular and humoral immunity is impacted in patients with ILD in the presence of immune disorders and immunosuppressive therapy. This results in poor control of viral infections following SARS-CoV-2 infection. We aimed to highlight the clinical management of patients with ILD with regard to the adjustment of anti-inflammatory therapy during SARS-CoV-2 infection.
We compared viral clearance, antibody levels, and T-cell immune response between healthy controls and patients with connective tissue disease-related ILD (CTD-ILD) or interstitial pneumonia with autoimmune features (IPAF).
Patients with ILD exhibited a higher viral load than the control group (1.58 × 106 vs. 2.37 × 103 copies/mL, p = 0.018), as well as a significantly lower level of neutralizing antibodies against the wild-type (WT) virus (7.01 vs. 625.6, p < 0.0001) and Omicron BA.5 (7.19 vs. 128.4, p < 0.001). Similarly, a lower virus-specific T-cell (VST) immune response was observed 14 days post-symptom onset in the ILD group (CD4+ VSTs: 0.018 vs. 0.082, p = 0.005; CD8+ VSTs: 0.0008 vs. 0.047, p = 0.004). The ILD group had no other heightened inflammatory biomarkers compared with the control group.
Our study provides novel evidence of the underlying interaction between virus clearance and host immune status and sheds light on the clinical management of patients with ILD with regard to the adjustment of anti-inflammatory therapy during SARS-CoV-2 infection.
Product Citations: 62
In Vaccines on 19 June 2025 by Zhong, J., Li, J., et al.
-
Immunology and Microbiology
In EBioMedicine on 1 May 2025 by van de Sandt, C. E., McQuilten, H. A., et al.
Susceptibility to life-threatening influenza increases with age, partly due to declining immunity. Frequency, phenotype and T-cell receptor (TCR) composition of influenza-specific CD8+ T-cells directed at the prominent A2/M158 influenza epitope change across the human lifespan.
We investigated longevity and mechanisms underlying age-related changes in influenza-specific TCR repertoires by performing longitudinal analyses in young and older adults across 7-12 years within A2/M158+CD8+ T-cells using peptide-HLA tetramers directly ex vivo. Paired TCRαβ-chains were used to track clonotypes over time within individuals.
Expanded public and private TCR clonotypes were long-lived but gradually declined over time. Loss of public clonotypes was initially compensated by expansions of clonotypes expressing public-associated features. Once these public-associated TCR clonotypes were abated in older adults, the void was filled by expansions of less similar private TCR clonotypes. Expanded older private TCR clonotypes also declined over time and were gradually replaced by other private TCR clonotypes with low similarity to public TCR clonotypes detected in adults.
Despite our relatively small cohort, we provided conclusive evidence that CD8+ T-cells to a single HLA-A2-restricted influenza-epitope are long-lived. However, dynamic changes occur at the clonotypic level, which eventually result in loss of public clonotypes, indicating that T-cell-based influenza vaccines are likely more effective in adults than older adults.
This research was supported by the National Health and Medical Research Council (#1173871, #1159272), the Australian Research Council (#190102704), European Union's Horizon 2020 (#792532), the University of Melbourne. Funders had no role in design, analysis or reporting of the study.
Copyright © 2025 The Author(s). Published by Elsevier B.V. All rights reserved.
-
Immunology and Microbiology
The Efficacy of Targeted Monoclonal IgA Antibodies Against Pancreatic Ductal Adenocarcinoma.
In Cells on 24 April 2025 by Raymakers, L., Passchier, E. M., et al.
The efficacy of immunotherapy in pancreatic ductal adenocarcinoma (PDAC) remains limited. The tumor microenvironment (TME), characterized by the accumulation of suppressive myeloid cells including neutrophils, attributes to immunotherapy resistance in PDAC. IgA monoclonal antibodies (mAbs) can activate neutrophils to kill tumor cells; this can be further enhanced by blocking the myeloid immune checkpoint CD47. In this study, we investigated the potential of this therapeutic strategy for PDAC. We determined the expression of tumor-associated antigens (TAAs) on PDAC cell lines and fresh patient samples, and the results showed that the TAAs epithelial cell adhesion molecule (EpCAM), trophoblast cell surface antigen 2 (TROP2) and mucin-1 (MUC1), as well as CD47 were consistently expressed on PDAC. In line with this, we showed that IgA mAbs against EpCAM can activate neutrophils to lyse various PDAC cell lines and tumor cells, which can be augmented by addition of CD47 blockade. In addition, we observed that neutrophils were present in patient tumors and expressed the receptor for IgA. In conclusion, our results indicate that a combination of IgA mAb with CD47 blockade is a promising preclinical treatment strategy for PDAC, which merits further investigation.
-
Cancer Research
-
Cell Biology
In Clinical Translational Immunology on 28 January 2025 by Messina, N. L., Germano, S., et al.
Bacille Calmette-Guérin (BCG) vaccination has off-target effects on disease risk for unrelated infections and immune responses to vaccines. This study aimed to determine the immunomodulatory effects of BCG vaccination on immune responses to vaccines against SARS-CoV-2.
Blood samples, from a subset of 275 SARS-CoV-2-naïve healthcare workers randomised to BCG vaccination (BCG group) or no BCG vaccination (Control group) in the BRACE trial, were collected before and 28 days after the primary course (two doses) of ChAdOx1-S (Oxford-AstraZeneca) or BNT162b2 (Pfizer-BioNTech) vaccination. SARS-CoV-2-specific antibodies were measured using ELISA and multiplex bead array, whole blood cytokine responses to γ-irradiated SARS-CoV-2 (iSARS) stimulation were measured by multiplex bead array, and SARS-CoV-2-specific T-cell responses were measured by activation-induced marker and intracellular cytokine staining assays.
After randomisation (mean 11 months) but prior to COVID-19 vaccination, the BCG group had lower cytokine responses to iSARS stimulation than the Control group. After two doses of ChAdOx1-S, differences in iSARS-induced cytokine responses between the BCG group and Control group were found for three cytokines (CTACK, TRAIL and VEGF). No differences were found between the groups after BNT162b2 vaccination. There were also no differences between the BCG and Control groups in COVID-19 vaccine-induced antigen-specific antibody responses, T-cell activation or T-cell cytokine production.
BCG vaccination induced a broad and persistent reduction in ex vivo cytokine responses to SARS-CoV-2. Following COVID-19 vaccination, this effect was abrogated, and BCG vaccination did not influence adaptive immune responses to COVID-19 vaccine antigens.
© 2025 The Author(s). Clinical & Translational Immunology published by John Wiley & Sons Australia, Ltd on behalf of Australian and New Zealand Society for Immunology, Inc.
-
COVID-19
-
Immunology and Microbiology
Cervical mucosal inflammation expands functional polymorphonuclear myeloid-derived suppressor cells
Preprint on MedRxiv : the Preprint Server for Health Sciences on 10 July 2024 by Pieren, D. K., Benítez-Martínez, A., et al.
The mucosal immune system plays a fundamental role in maintaining microbial balance. Microbial imbalance in the female genital tract increases the risk for adverse health outcomes in women and may increase susceptibility to genital tract infections. Among different relevant immune subsets, myeloid-derived suppressor cells (MDSCs) remain understudied in the context of female genital tract conditions. Here we show that frequency of polymorphonuclear (PMN-) MDSCs increased in the cervical mucosa of women with Chlamydia trachomatis , bacterial vaginosis, or with a coinfection, but not in women with human papillomavirus. Mucosal PMN-MDSC frequencies correlated with mucosal IL-1β in C. trachomatis patients and ex vivo exposure of cervical tissue to C. trachomatis elevated both PMN-MDSC frequencies and IL-1β secretion. Likewise, exposure of cervical tissue to cervicovaginal lavage fluid from C. trachomatis and bacterial vaginosis patients also enhanced PMN-MDSC frequencies. Lastly, cervical MDSCs expressed suppressive mediators and functionally suppressed cytotoxic T-cell responses. Our study identifies IL-1β-stimulated PMN-MDSCs as an immune suppressive mediator in female genital tract infections, potentially contributing to susceptibility to acquiring secondary infections at this site.
-
FC/FACS
-
Immunology and Microbiology
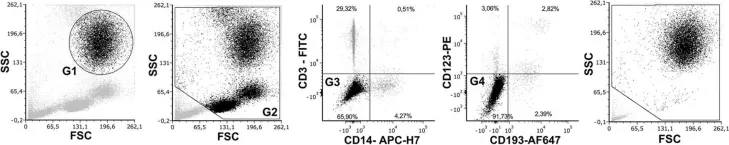
In Front Immunol on 17 May 2018 by Bastian, O. W., Croes, M., et al.
Fig.1.A

-
FC/FACS
-
Homo sapiens (Human)
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 2
In Front Immunol on 17 May 2018 by Bastian, O. W., Croes, M., et al.
Fig.1.B

-
FC/FACS
-
Homo sapiens (Human)
Collected and cropped from Front Immunol by CiteAb, provided under a CC-BY license
Image 1 of 2