Limited immune infiltration within the tumor microenvironment (TME) hampers the efficacy of immune checkpoint blockade (ICB) therapy. To enhance immune infiltration, mild photothermal therapy (PTT) is often combined with immunotherapy. However, the impact of mild PTT on the TME remains unclear. The bioinformatics analyses reveal that mild PTT amplifies immune cell infiltration and stimulates T-cell activity. Notably, it accelerates the release of tumor cell-derived exosomes (TEX) and upregulates PD-L1 expression on both tumor cells and TEX. Consequently, it is proposed that locally inhibiting TEX release is crucial for overcoming the adverse effects of mild PTT, thereby enhancing ICB therapy. Thus, a multi-stage drug delivery system is designed that concurrently delivers photosensitizers (reduced graphene oxide nanosheets, NRGO), anti-PD-L1 antibodies, and exosome inhibitors (sulfisoxazole). The system employs a temperature-sensitive lipid gel as the primary carrier, with NRGO serving as a secondary carrier that supports photothermal conversion and incorporation of sulfisoxazole. Importantly, controlled drug release is achieved using near-infrared radiation. The findings indicate that this local combination therapy remodels the immunosuppressive TME through exosome inhibition and enhanced immune cell infiltration, while also boosting T-cell activity to trigger systemic antitumor immunity, showcasing the remarkable efficacy of this combination strategy in eradicating cold tumors.
© 2024 The Author(s). Advanced Science published by Wiley‐VCH GmbH.
Product Citations: 36
Local Exosome Inhibition Potentiates Mild Photothermal Immunotherapy Against Breast Cancer.
In Advanced Science (Weinheim, Baden-Wurttemberg, Germany) on 1 January 2025 by Chen, Q., Li, Y., et al.
-
Cancer Research
-
Immunology and Microbiology
In eLife on 22 November 2024 by Garnica, J., Solé, P., et al.
Chronic antigenic stimulation can trigger the formation of interleukin 10 (IL-10)-producing T-regulatory type 1 (TR1) cells in vivo. We have recently shown that murine T-follicular helper (TFH) cells are precursors of TR1 cells and that the TFH-to-TR1 cell transdifferentiation process is characterized by the progressive loss and acquisition of opposing transcription factor gene expression programs that evolve through at least one transitional cell stage. Here, we use a broad range of bulk and single-cell transcriptional and epigenetic tools to investigate the epigenetic underpinnings of this process. At the single-cell level, the TFH-to-TR1 cell transition is accompanied by both, downregulation of TFH cell-specific gene expression due to loss of chromatin accessibility, and upregulation of TR1 cell-specific genes linked to chromatin regions that remain accessible throughout the transdifferentiation process, with minimal generation of new open chromatin regions. By interrogating the epigenetic status of accessible TR1 genes on purified TFH and conventional T-cells, we find that most of these genes, including Il10, are already poised for expression at the TFH cell stage. Whereas these genes are closed and hypermethylated in Tconv cells, they are accessible, hypomethylated, and enriched for H3K27ac-marked and hypomethylated active enhancers in TFH cells. These enhancers are enriched for binding sites for the TFH and TR1-associated transcription factors TOX-2, IRF4, and c-MAF. Together, these data suggest that the TR1 gene expression program is genetically imprinted at the TFH cell stage.
© 2024, Garnica et al.
In British Journal of Pharmacology on 1 November 2024 by Ruixin, S., Yifan, L., et al.
Although our previous data indicated that claudin 18 isoform 2 (CLDN18.2)-targeted chimeric antigen receptor (CAR) T cells displayed remarkable clinical efficacy in CLDN18.2-positive gastric cancer, their efficacy is limited in pancreatic ductal adenocarcinoma (PDAC). The tumour microenvironment (TME) is one of the main obstacles to the efficacy of CAR-T and remodelling the TME may be a possible way to overcome this obstacle. The TME of PDAC is characterized by abundant cancer-related fibroblasts (CAFs), which hinder the infiltration and function of CLDN18.2-targeted CAR-T cells. The expression of fibroblast activation protein alpha (FAP) is an important feature of active CAFs, providing potential targets for eliminating CAFs.
In this study, we generated 10 FAP/CLDN 18.2 dual-targeted CAR-T cells and evaluated their anti-tumour ability in vitro and in vivo.
Compared with conventional CAR-T cells, some dual-targeted CAR-T cells showed improved therapeutic effects in mouse pancreatic cancers. Further, dual-targeted CAR-T cells with better anti-tumour effect could suppress the recruitment of myeloid-derived suppressor cells (MDSCs) to improve the immunosuppressive TME, which contributes to the survival of CD8+ T cells. Moreover, dual-targeted CAR-T cells reduced the exhaustion of T cells in transforming TGF-β dependent manner.
The dual-targeted CAR-T cells obtained enhancement of T effector function, inhibition of T cell exhaustion, and improvement of tumour microenvironment. Our findings provide a theoretical rationale for dual-targeted FAP/CLDN 18.2 CAR-T cells therapy in PDAC.
© 2024 British Pharmacological Society.
-
Mus musculus (House mouse)
-
Cancer Research
-
Immunology and Microbiology
-
Pharmacology
Effects of PACAP Deficiency on Immune Dysfunction and Peyer's Patch Integrity in Adult Mice.
In International Journal of Molecular Sciences on 3 October 2024 by Sparks, J., Meggyes, M., et al.
PACAP (pituitary adenylate cyclase activating polypeptide) is a widespread neuropeptide with cytoprotective and anti-inflammatory effects. It plays a role in innate and adaptive immunity, but data are limited about gut-associated lymphoid tissue. We aimed to reveal differences in Peyer's patches between wild-type (WT) and PACAP-deficient (KO) mice. Peyer's patch morphology from young (3-months-old) and aging (12-15-months-old) mice was examined, along with flow cytometry to assess immune cell populations, expression of checkpoint molecules (PD-1, PD-L1, TIM-3, Gal-9) and functional markers (CD69, granzyme B, perforin) in CD3+, CD4+, and CD8+ T cells. We found slight differences between aging, but not in young, WT, and KO mice. In WT mice, aging reduced CD8+ T cell numbers frequency and altered checkpoint molecule expression (higher TIM-3, granzyme B; lower Gal-9, CD69). CD4+ T cell frequency was higher with similar checkpoint alterations, indicating a regulatory shift. In PACAP KO mice, aging did not change cell population frequencies but led to higher TIM-3, granzyme B and lower PD-1, PD-L1, Gal-9, and CD69 expression in CD4+ and CD8+ T cells, with reduced overall T cell activity. Thus, PACAP deficiency impacts immune dysfunction by altering checkpoint molecules and T cell functionality, particularly in CD8+ T cells, suggesting complex immune responses by PACAP, highlighting its role in intestinal homeostasis and potential implications for inflammatory bowel diseases.
-
Mus musculus (House mouse)
-
Immunology and Microbiology
Macrophage-mediated myelin recycling fuels brain cancer malignancy.
In Cell on 19 September 2024 by Kloosterman, D. J., Erbani, J., et al.
Tumors growing in metabolically challenged environments, such as glioblastoma in the brain, are particularly reliant on crosstalk with their tumor microenvironment (TME) to satisfy their high energetic needs. To study the intricacies of this metabolic interplay, we interrogated the heterogeneity of the glioblastoma TME using single-cell and multi-omics analyses and identified metabolically rewired tumor-associated macrophage (TAM) subpopulations with pro-tumorigenic properties. These TAM subsets, termed lipid-laden macrophages (LLMs) to reflect their cholesterol accumulation, are epigenetically rewired, display immunosuppressive features, and are enriched in the aggressive mesenchymal glioblastoma subtype. Engulfment of cholesterol-rich myelin debris endows subsets of TAMs to acquire an LLM phenotype. Subsequently, LLMs directly transfer myelin-derived lipids to cancer cells in an LXR/Abca1-dependent manner, thereby fueling the heightened metabolic demands of mesenchymal glioblastoma. Our work provides an in-depth understanding of the immune-metabolic interplay during glioblastoma progression, thereby laying a framework to unveil targetable metabolic vulnerabilities in glioblastoma.
Copyright © 2024 The Authors. Published by Elsevier Inc. All rights reserved.
-
Mus musculus (House mouse)
-
Cancer Research
-
Immunology and Microbiology
-
Neuroscience
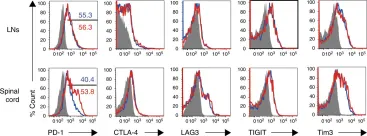
In Nat Commun on 1 February 2019 by Yasuda, K., Kitagawa, Y., et al.
Fig.6.A

-
FC/FACS
-
Mus musculus (House mouse)
Collected and cropped from Nat Commun by CiteAb, provided under a CC-BY license
Image 1 of 1