One of the most used chemotherapy agents in clinical practice is 5-Fluorouracil (5-FU), a fluorinated pyrimidine in the category of antimetabolite agents. 5-FU is used to treat a variety of cancers, including colon, breast, pancreatic, and stomach cancers, and its efficacy lies in its direct impact on the patient's DNA and RNA. Specifically, its mechanism blocks the enzymes thymidylate synthetase and uracil phosphatase, inhibiting the synthesis of uracil, which cannot be incorporated into nuclear and cytoplasmic RNA. Despite being one of the most used drugs in oncology, it is associated with several significant side effects, including inflammation of the mouth, loss of appetite, and reduction in blood cells. In our study, we examined the reduction of side effects in a 5-FU regimen administered at doses of 15 mg/kg and 6 mg/kg for 14 days in 6-week-old male Sprague-Dawley rats. On the 14th day, the rats were treated orally for 2 weeks with 100 mg/kg of Ulva pertusa, a well-known seaweed from the Ulvaceae family, which has demonstrated powerful biological properties. The administration of this green alga alleviated the side effects of 5-FU, improving several parameters including body weight, food intake, and diarrhea index. It also helped reduce side effects in the blood, kidneys, and liver. Histological and molecular analyses were conducted on serum and colon tissues from the rats, examining changes in colon structure and the release of oxidative stress markers such as iNOS, COX-2, and nitrotyrosine. Several biochemical indicators, including SOD, CAT, GSH, MDA, and ascorbic acid, were also evaluated. Overall, our data indicated Ulva pertusa to be a promising therapeutic against 5-FU's adverse effects, therefore, it could be worthwhile to investigate the possibility of using this alga in safer cancer treatment formulations. Certainly, future preclinical and clinical studies could assess the alga's efficacy in diverse cancer treatment regimens, exploring its role as an adjuvant therapy that may reduce chemotherapy-related toxicity without compromising therapeutic outcomes.
Product Citations: 60
In International Journal of Molecular Sciences on 3 December 2024 by Repici, A., Capra, A. P., et al.
Inhibiting CD44-ICD Attenuates LPS-Induced Initiation of Hepatic Inflammation in Septic Mice.
In International Journal of Molecular Sciences on 15 August 2024 by Li, L. H., Hsu, D. Z., et al.
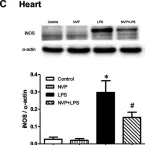
Sepsis is a severe condition induced by microbial infection. It elicits a systemic inflammatory response, leading to multi-organ failure, and the liver, as a scavenger, plays a significant role in this process. Controlling hepatic inflammation and maintaining liver function is crucial in managing sepsis. CD44-ICD, as a CD44 signal transductor, is involved in multiple inflammatory responses. However, the role of CD44-ICD in lipopolysaccharide (LPS)-induced hepatic inflammation has not been investigated. Therefore, we aimed to examine whether CD44-ICD initiates hepatic inflammation in septic mice. We induced hepatic inflammation in mice by administering LPS. DAPT, a CD44-ICD inhibitor, was given to mice or Chang cells 30 min or 1 h before LPS administration (10 mg/kg, i.p., or 100 ng/mL, respectively). Inhibition of CD44-ICD decreased the level of aspartate aminotransferase (AST), alanine aminotransferase (ALT), hepatic necrosis, inflammatory cell infiltration, interleukin (IL)-1β, inducible NO synthase (iNOS), nitric oxide (NO) production, nuclear factor (NF)κB signaling pathway proteins, and CD44 expression in mice. CD44-ICD inhibition also decreased IL-1β and CD44 expression levels in Chang cells. CD44-ICD may be a primary regulatory function in CD44-associated LPS-induced initiation of hepatic inflammation in mice.
-
Mus musculus (House mouse)
-
Immunology and Microbiology
In Cells on 15 May 2024 by Seoane, N., Picos, A., et al.
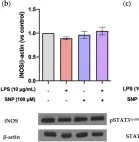
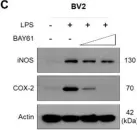
In various neurodegenerative conditions, inflammation plays a significant role in disrupting the blood-brain barrier (BBB), contributing to disease progression. Nitric oxide (NO) emerges as a central regulator of vascular function, with a dual role in inflammation, acting as both a pro- and anti-inflammatory molecule. This study investigates the effects of the NO donor sodium nitroprusside (SNP) in protecting the BBB from lipopolysaccharide (LPS)-induced inflammation, using bEnd.3 endothelial cells as a model system. Additionally, Raw 264.7 macrophages were employed to assess the effects of LPS and SNP on their adhesion to a bEnd.3 cell monolayer. Our results show that LPS treatment induces oxidative stress, activates the JAK2/STAT3 pathway, and increases pro-inflammatory markers. SNP administration effectively mitigates ROS production and IL-6 expression, suggesting a potential anti-inflammatory role. However, SNP did not significantly alter the adhesion of Raw 264.7 cells to bEnd.3 cells induced by LPS, probably because it did not have any effect on ICAM-1 expression, although it reduced VCAM expression. Moreover, SNP did not prevent BBB disruption. This research provides new insights into the role of NO in BBB disruption induced by inflammation.
-
WB
-
Mus musculus (House mouse)
-
Cardiovascular biology
-
Cell Biology
-
Immunology and Microbiology
In International Journal of Molecular Sciences on 14 April 2024 by Repici, A., Capra, A. P., et al.
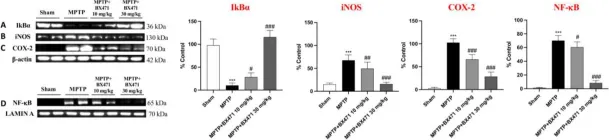
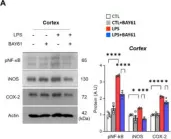
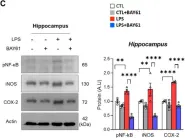
Parkinson's disease (PD) is recognized as the second most common neurodegenerative disease worldwide. Even if PD etiopathogenesis is not yet fully understood, in recent years, it has been advanced that a chronic state of inflammation could play a decisive role in the development of this pathology, establishing the close link between PD and neuroinflammation. In the broad panorama of inflammation and its several signaling pathways, the C-C chemokine receptor type 1 (CCR1) could play a key pathogenic role in PD progression, and could constitute a valuable target for the development of innovative anti-PD therapies. In this study, we probed the neuroprotective properties of the CCR1 antagonist BX471 compound in a mouse model of MPTP-induced nigrostriatal degeneration. BX471 treatments were performed intraperitoneally at a dose of 3 mg/kg, 10 mg/kg, and 30 mg/kg, starting 24 h after the last injection of MPTP and continuing for 7 days. From our data, BX471 treatment strongly blocked CCR1 and, as a result, decreased PD features, also reducing the neuroinflammatory state by regulating glial activation, NF-κB pathway, proinflammatory enzymes, and cytokines overexpression. Moreover, we showed that BX471's antagonistic action on CCR1 reduced the infiltration of immune cells, including mast cells and lymphocyte T activation. In addition, biochemical analyses carried out on serum revealed a considerable increase in circulating levels of CCR1 following MPTP-induced PD. In light of these findings, CCR1 could represent a useful pathological marker of PD, and its targeting could be a worthy candidate for the future development of new immunotherapies against PD.
-
WB
-
Mus musculus (House mouse)
-
Neuroscience
In Molecular Nutrition Food Research on 14 February 2024 by Fan, H., Shang, N., et al.
This study aims to investigate the antihypertensive effect of four chicken muscle-derived angiotensin (Ang)-converting enzymes (ACE)-regulating peptides: Val-Arg-Pro (VRP, ACE inhibition), Leu-Lys-Tyr and Val-Arg-Tyr (LKY and VRY, ACE inhibition and ACE2 upregulation), and Val-Val-His-Pro-Lys-Glu-Ser-Phe (VVHPKESF [V-F], ACE2 upregulation) in spontaneously hypertensive rats.
Rats (12-14 weeks old) are grouped: 1) untreated, 2) VRP, 3) LKY, 4) VRY, and 5) V-F. Blood pressure (BP) is monitored using implantable telemetry technology. Over 18-day oral administration of 15 mg kg-1 body weight (BW) per day, only peptide V-F significantly (p < 0.05) reduces BP, decreases circulating Ang II, and increases ACE2 and Ang (1-7) levels, and enhances aortic expressions of ACE2 and Mas receptor (MasR). Peptide V-F also attenuates vascular inflammation (TNFα, MCP-1, IL-1α, IL-15, and cyclooxygenase 2 [COX2]) and vascular oxidative stress (nitrotyrosine). The gastrointestinal (GI)-degraded fragment of peptide V-F, Val-Val-His-Pro-Lys (VVHPK), is also an ACE2-upregulating peptide. Peptides VRP, LKY, and VRY do not reduce BP, possibly due to low bioavailability or other unknown reasons.
Peptide V-F is the first ACE2-upregulating peptide, purified and fractionated from food proteins based on in vitro ACE2 upregulation, that reduces BP associated with the activation of ACE2/Ang (1-7)/MasR axis; the N-terminal moiety VVHPK may be responsible for the antihypertensive effect of V-F.
© 2024 Wiley-VCH GmbH.
-
Cardiovascular biology
-
Veterinary Research
In Cells on 15 May 2024 by Seoane, N., Picos, A., et al.
Fig.5.B

-
WB
-
Mus musculus (House mouse)
Collected and cropped from Cells by CiteAb, provided under a CC-BY license
Image 1 of 10
In Int J Mol Sci on 14 April 2024 by Repici, A., Capra, A. P., et al.
Fig.6.A

-
WB
-
Mus musculus (House mouse)
Collected and cropped from Int J Mol Sci by CiteAb, provided under a CC-BY license
Image 1 of 10
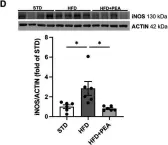
In Front Nutr on 21 August 2023 by Pirozzi, C., Coretti, L., et al.
Fig.2.D

-
WB
-
Mus musculus (House mouse)
Collected and cropped from Front Nutr by CiteAb, provided under a CC-BY license
Image 1 of 10
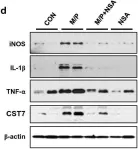
In Sci Rep on 31 May 2023 by Leem, Y. H., Kim, D. Y., et al.
Fig.6.D

-
WB
-
Mus musculus (House mouse)
Collected and cropped from Sci Rep by CiteAb, provided under a CC-BY license
Image 1 of 10
In J Clin Med on 25 July 2022 by A, A., Filippone, A., et al.
Fig.4.A

-
WB
-
Collected and cropped from J Clin Med by CiteAb, provided under a CC-BY license
Image 1 of 10
In Cells on 28 May 2022 by Kim, M. W., Choe, K., et al.
Fig.3.A

-
WB
-
Mus musculus (House mouse)
Collected and cropped from Cells by CiteAb, provided under a CC-BY license
Image 1 of 10
In Cells on 28 May 2022 by Kim, M. W., Choe, K., et al.
Fig.3.C

-
WB
-
Mus musculus (House mouse)
Collected and cropped from Cells by CiteAb, provided under a CC-BY license
Image 1 of 10
In Cells on 28 May 2022 by Kim, M. W., Choe, K., et al.
Fig.4.C

-
WB
-
Mus musculus (House mouse)
Collected and cropped from Cells by CiteAb, provided under a CC-BY license
Image 1 of 10
In Front Pharmacol on 24 August 2021 by Liu, P. Y., Shen, H. H., et al.
Fig.4.C

-
WB
-
Collected and cropped from Front Pharmacol by CiteAb, provided under a CC-BY license
Image 1 of 10
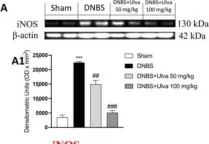
In Antioxidants (Basel) on 3 September 2020 by Siracusa, R., Scuto, M., et al.
Fig.8.A

-
WB
-
Collected and cropped from Antioxidants (Basel) by CiteAb, provided under a CC-BY license
Image 1 of 10